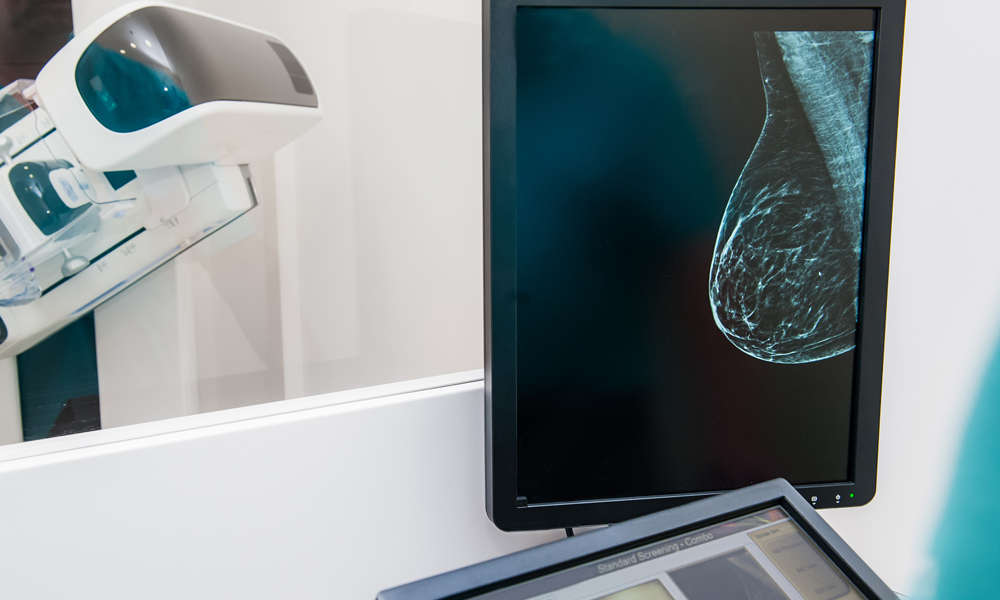
Whenever women have an operation for breast cancer, surgeons routinely check the armpit to see if cancer has spread to the lymph nodes. This is called a sentinel lymph node biopsy. Blue dye is injected into the breast at the time of surgery. The dye then travels into the armpit, and turns an average of two nodes bright blue – these are the sentinel nodes that get removed for further testing and will reveal whether or not cancer has spread from the breast to the lymph nodes.
A prophylactic mastectomy – such as the one that Angelina Jolie underwent at the Pink Lotus Breast Center in 2013 – means removing a breast that has no known disease within it. Since the removal of the breast is prophylactic, the trend has historically been not to perform a sentinel node biopsy. If you were having a prophylactic mastectomy, would you want your sentinel node checked for cancer?
The rate of cancer found incidentally within the breast after a prophylactic mastectomy ranges from 2-8%.[i] [ii] [iii] [iv] [v][vi] [vii] When cancer is indeed found after the mastectomy, a sentinel node biopsy is no longer possible given that there is no longer a breast into which dye can be injected. Therefore, women choosing to have a prophylactic mastectomy (whether for a BRCA gene mutation or other reason) must consider that 2-8% risk and decide if they want a sentinel node biopsy or not.
Why the dilemma? Well, sentinel node biopsies can have complications, such as pain, numbness, arm swelling (lymphedema), fluid buildup (seroma), limited arm movement, and infection. Since about 95% of patients having a prophylactic mastectomy do not have cancer found in the breast, most women do not want to take the additional risks associated with a sentinel node biopsy. However, if cancer is found in the breast after removal and a sentinel node biopsy was not chosen, all armpit nodes would need to be removed in order to see if any of them shows signs of cancer. While this is the only way to assure that no cancer has spread beyond the breast, removal of all those nodes causes complications in up to 84% of patients [viii] [ix] [x] versus 10% for a sentinel node.[xi] [xii] To use an example of the most feared complication of axillary surgery, lymphedema occurs in 2% after sentinel biopsy, and in 13% after complete dissection.[xiii] Finding out whether cancer escaped to the nodes is critical, because positive nodes can significantly alter the need for additional treatments such as chemotherapy, hormonal therapy, and radiation.
Over 11 hours of video content are now available to stream from any device. If you cannot attend our annual Summit at Terranea Resort, sign up for the Virtual Summit instead and get the same information from the in-person Summit in the convenience of your own home.
So, would you choose a sentinel node biopsy as an “insurance policy” against needing a more invasive axillary procedure if cancer is found in your breast after removal? Again, the trend has historically been not to perform sentinel node biopsy during prophylactic mastectomy, except in the setting of a locally advanced cancer in the opposite breast.[iv] [v] [vi] [vii] If you fall within the 5% of women who have cancer found after a prophylactic mastectomy, removal of all the nodes is the only generally accepted method to rule out spread.
This predicament has a practical solution invented by Dr. Kristi Funk, who performed Jolie’s procedure. Dr. Funk has used her new technique, called Prophylactic Breast Dye Injection (PBDI), at the Pink Lotus Breast Center since February 2013. Blue dye is injected into the breast at the time of a prophylactic mastectomy, but no lymph nodes are removed during the procedure (unless the patient has selected to do so), in hopes that no cancer will be found after removal of the breast. Yet, if cancer is found within the tissue after Pathology analyzes the entire breast (this usually takes several days), the sentinel nodes in question will still be bright blue from the procedure days earlier since the dye takes weeks to months to be cleared out of your system. Therefore, the surgeon simply returns to the operating room for a quick procedure to remove the blue sentinel nodes – avoiding a complete dissection of the armpit.
Prophylactic Breast Dye Injection (PBDI) eliminates the stressful choice of: “I am having a prophylactic mastectomy. Do I take the node or not?” Dr. Funk’s innovative solution is to take the sentinel nodes when they are needed, after-the-fact, and to leave them alone if the breast is benign. PBDI provides women with peace of mind and control – two critical elements of Dr. Funk’s mission and the philosophy that has been incorporated into her Pink Lotus Breast Center.
Disclaimer: While PBDI has been used successfully over the past many years, it is unknown which factors influence the precise length of time that the blue dye remains in the sentinel nodes. Further studies in that regard are needed.
Stay Connected
Stay Connected
References
- Dupont EL, Kuhn MA, McCann C, et al: The role of sentinel lymph node biopsy in women undergoing prophylactic mastectomy. Am J Surg 180:274-277, 2000.
- Geiger AM, Yu O, Herrinton LJ, et al. A Population-Based Study of Bilateral Prophylactic Mastectomy Efficacy in Women at Elevated Risk for Breast Cancer in Community Practices. Arch Intern Med. 2005;165(5):516-520. doi:10.1001/archinte.165.5.516.
- Contralateral prophylactic mastectomy improves the outcome of selected patients undergoing mastectomy for breast cancer. E A EA Peralta, J D JD Ellenhorn, L D LD Wagman, A A Dagis, J S JS Andersen, D Z DZ Chu Am J Surg 180(6):439-45 (2000)
- Zhou, Wen-Bin, et al. “Meta-analysis of sentinel lymph node biopsy at the time of prophylactic mastectomy of the breast.” Canadian Journal of Surgery 54.5 (2011): 300.
- Nasser, Samiha M., Savanna G. Smith, and Anees B. Chagpar. “The role of sentinel node biopsy in women undergoing prophylactic mastectomy.” Journal of Surgical Research 164.2 (2010): 188-192.
- Czyszczon, Irene Alina, Lane Roland, and Sunati Sahoo. “Routine prophylactic sentinel lymph node biopsy is not indicated in women undergoing prophylactic mastectomy.” Journal of surgical oncology (2012).
- Laronga, Christine, et al. “Indications for sentinel lymph node biopsy in the setting of prophylactic mastectomy.” Journal of the American College of Surgeons 209.6 (2009): 746-752.
- Warmuth MA, Bowen G, Prosnitz LR et al. Complications of axillary lymph node dissection for carcinoma of the breast: a report based on a patient survey. Cancer 1998; 83:1362-8.
- Ivens D, Hoe AL, Podd TJ, Hamilton CR, Taylor I, Royle GT. Assessment of morbidity from complete axillary dissection. Br J Cancer. 1992;66(1):136-138
- Yeoh EK, Denham JW, Davies SA, Spittle MF. Primary breast cancer: complications of axillary management. Acta Radiol Oncol. 1986;25(2):105-108
- Wilke, Lee Gravatt, et al. “Surgical complications associated with sentinel lymph node biopsy: results from a prospective international cooperative group trial.” Annals of surgical oncology 13.4 (2006): 491-500.
- Mansel RE, Fallowfield L, Kissin M, et al. Randomized Multicenter Trial of Sentinel Node Biopsy Versus Standard Axillary Treatment in Operable Breast Cancer: The ALMANAC Trial. Journal of the National Cancer Institute 2006 May 3;98(9):599–609.
- Lucci A, McCall LM, Beitsch PD, et al. Surgical complications associated with sentinel lymph node dissection (SLND) plus axillary lymph node dissection compared with SLND alone in the American College of Surgeons Oncology Group Trial Z0011. J Clin Oncol 2007; 25:3657.