What is MRI technology, how does it work, and under what circumstances should it be considered? Here are some quick facts on MRI.
What is an MRI?
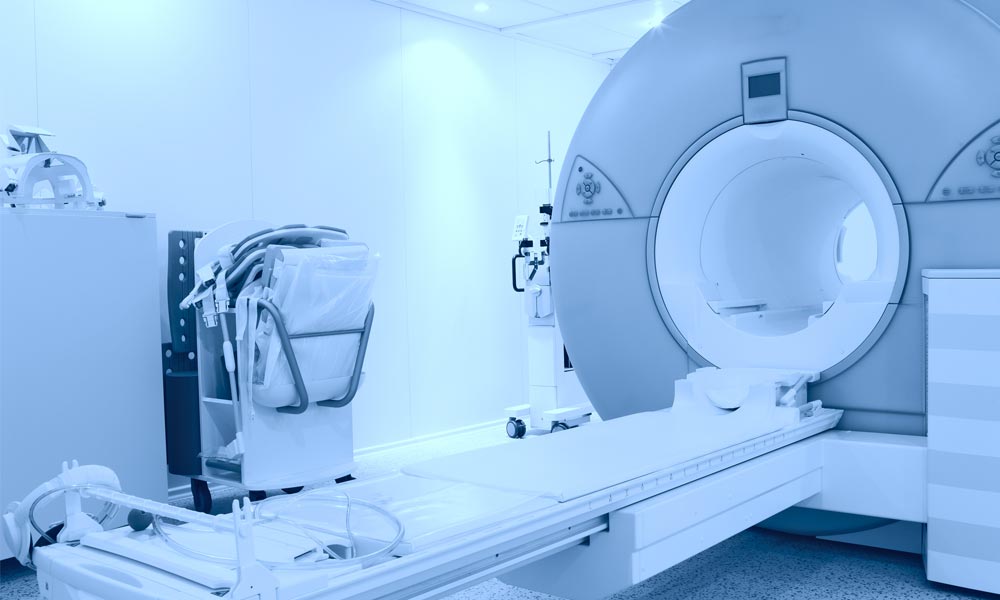
Magnetic Resonance Imaging (MRI) combines radio waves and a strong magnetic field (not radiation) to produce three dimensional images of the breast. A woman lies face-down on a table, with both breasts falling through an opening in the table (this allows more breast tissue to be seen than when lying face-up).
The table then moves the patient in and out of a tube which generates images of the breasts. Contrast dye (gadolinium) injected into a patient’s vein highlights abnormalities in the breast based on blood flow patterns. Abnormalities appear brighter than the background breast tissue and allow the radiologist to study these areas more closely. The exam takes about 45 minutes, and can be difficult for claustrophobic patients. Also, those with non-titanium metal in their bodies cannot have an MRI.
Over 11 hours of video content are now available to stream from any device. If you cannot attend our annual Summit at Terranea Resort, sign up for the Virtual Summit instead and get the same information from the in-person Summit in the convenience of your own home.
Who should get an MRI?
There are many circumstances under which an MRI should be considered. For instance, newly diagnosed cancer patients should generally get an MRI to evaluate the extent of disease in the affected breast, as well as to check for cancer in the opposite breast. Also, known BRCA carriers and patients with a lifetime breast cancer risk exceeding 20% are often candidates for an MRI. Other reasons to get an MRI can include an abnormal mammogram or breast ultrasound with MRI recommended by a radiologist, a history of radiation to the chest before age 30, a suspicion of leaking silicone implants, or other indications determined by a physician.
Stay Connected
Stay Connected
Shouldn’t everyone get an MRI?
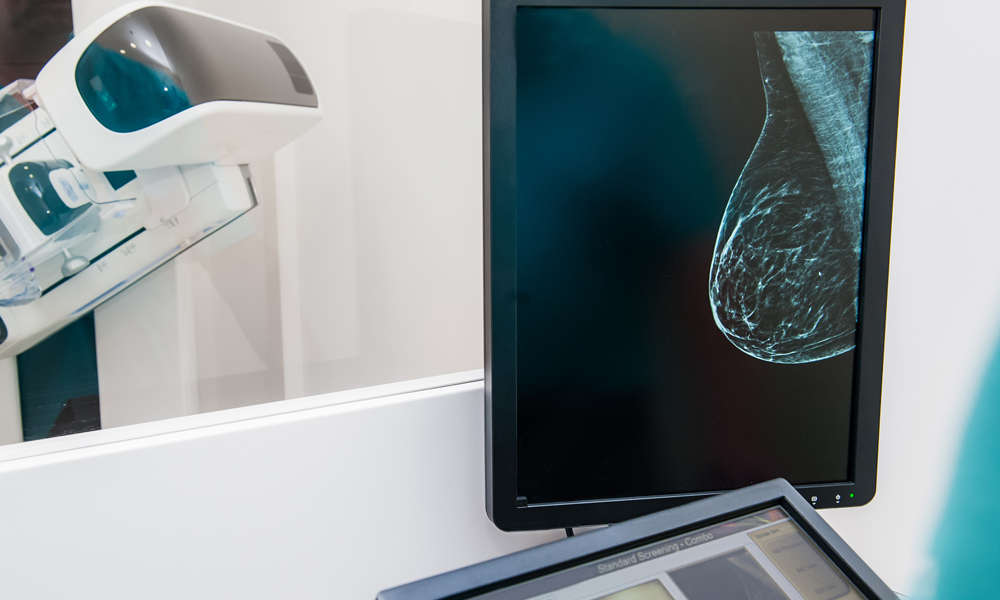
Screening MRIs, meant to evaluate healthy tissue for hidden cancers, are not currently recommended for normal risk women. Mammograms remain the gold standard for screening women at average risk for developing breast cancer.