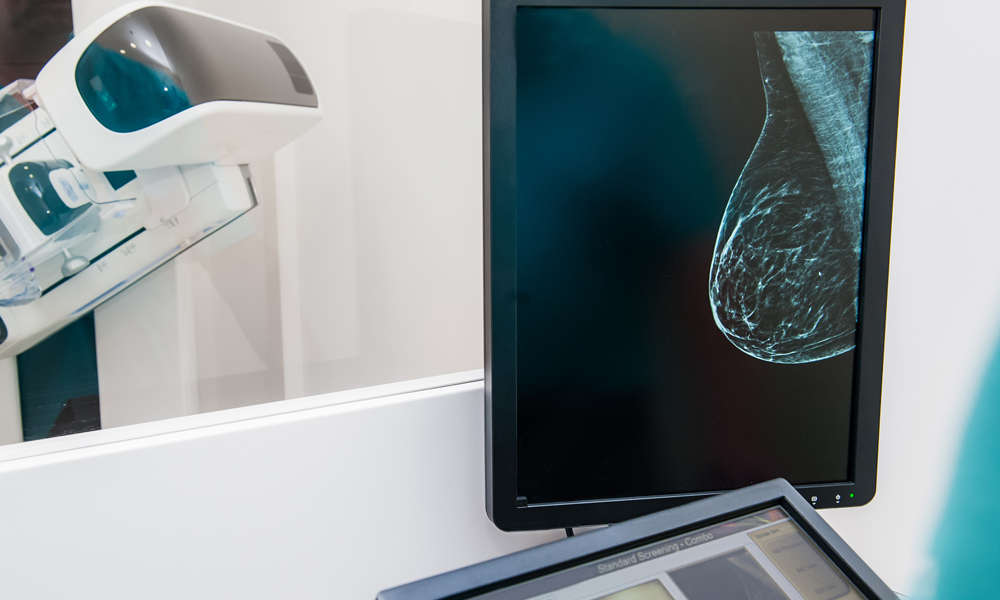
Your pathology report reveals the results of your breast cancer biopsy. These answers may take between one and two weeks to be completed depending on the type of biopsy you had and where you are being treated. It is one of the most important documents you will receive during the course of your diagnosis. It contains a complete profile of the cancer’s characteristics. It describes features that enable your doctor to see how aggressive the tumor is. From the results detailed in the pathology report, your doctor will be able to make suggestions about what treatments will be best in order to hopefully cure your cancer.
When you receive your breast cancer pathology report, you will probably feel a little overwhelmed as it contains a lot of information, and some of it may be difficult to interpret. Going over the report with your doctor will help things appear much clearer. The following general guideline should help you to read your pathology report and to understand some of the terminology you may come across.
Breast Cancer Type
Identifying the type of cancer is a crucial step for deciding on treatment because not all types of cancer are treated the same. For example, a treatment for carcinoma will not work on lymphoma. All breast cancers coming from breast cells are adenocarcinomas.
Ductal vs. Lobular
About 75 percent of all breast cancers originate inside milk ducts (thin tubes that carry milk out the nipple), 10 percent begin in the milk-produding lobules, and 15 percent involve less common subtypes that usually also initiate in the ducts but have unique features about them that make them have other descriptive names like mucinous or tubular, but it’s all breast cancer.
Invasive vs. Non-Invasive
If the cancer is non-invasive, also called in-situ, this means that it has not broken through the milk ducts in the breast, and the duct wall is intact. If it is invasive, cancer cells have pushed through the duct wall (or the lobule, in the case of invasive lobular cancer), but this only means it has broken the duct wall in your breast, not that it has invaded your nodes or other organs (although it is possible that this has happened).
Over 11 hours of video content are now available to stream from any device. If you cannot attend our annual Summit at Terranea Resort, sign up for the Virtual Summit instead and get the same information from the in-person Summit in the convenience of your own home.
Grade
Grade can be called 1, 2, 3; low, intermediate, high; or well, moderately, poorly differentiated (it’s all the same).
These terms explain how aggressive the cancer is likely to be. Grade compares features of the cancer cell to a normal cell, giving us insight into how hostile the cells might be. Grade 1 looks similar to the original breast cell, grade 2 is more altered, and grade 3 appears wild. Bottom line: the higher the grade, the more aggressive the cancer.
Lymphovascular Invasion
This will show whether the breast cancer has spread to the lymphatic fluid channels. Additionally, some tumor types require extra analysis because they may benefit from targeted therapies. Hormonal markers can help your doctor decide which drugs may have the greatest impact.
Hormone Receptor Status
This test tells you whether or not the breast cancer cells contain estrogen or progesterone receptor cells. The presence or absence of hormone receptors greatly affects your treatment options. Having these receptors generally corresponds to less aggressive cancers.
Stay Connected
Stay Connected
HER2 Status
The HER2 gene can play a role in breast cancer. HER2-positive breast cancer indicates the presence of a protein known as human epidermal growth factor receptor 2, which stimulates the growth of cancer cells.
Rate of Cell Growth
Your pathology report may also include information about cell growth rate. This refers to the percentage of tumor cancer cells which are multiplying to produce new cancer cells. A higher proportion of cell growth translates to a more aggressive, faster-growing cancer. Several tests can be conducted to measure cell growth, such as:
- S-phase Fraction: The result of this tests tells you what percentage of cells in the tumor sample are reproducing their DNA. Less than 6 percent is considered low, while 6 -10 percent is intermediate, and 10 percent and above is considered high.
- Ki-67: This is a form of protein which increases when cells get ready to divide and form new cells. A result of less than 10 percent is considered low, 10-20 percent is considered borderline, and greater than 20 percent is considered high.
Lymph Node Status
This is a separate biopsy from the one on your breast, and if the nodes in your armpit appeared normal on imaging, there will be no reason to have biopsied them prior to surgery. If nodes were biopsied, then your report will state whether breast cancer cells were seen in the lymph nodes or not.
Not all pathology labs perform all of the above tests routinely, so they may or may not appear in your pathology report. You can always request that any missing tests be done on the existing biopsy (you do not have to repeat the biopsy).
Breast Cancer Staging
Breast cancer stages range from stage 0 (pre-invasive) to stage IV (cancer has spread beyond breast and axillary nodes into another organ in the body). Breast cancer staging uses the “TNM staging system” and is dependent upon three specific factors:
- Tumor (T): The size of the tumor.
- Lymph node: (N): Whether or not cancer has spread to the lymph nodes, and if so, how many.
- Metastasis (M): Whether the cancer has spread to other parts of the body, such as the bones or lungs.
A number will be assigned to each of these categories to indicate the extent of cancer development. These classifications will be combined to designate the stage of your breast cancer. The stage cannot be determined using only the information in your pathology report, as stage factors in the exact number of involved nodes and their locations, and also the possibility of spread to other organs, none of which is in your path report.
Stage 0 – Tis, N0, M0
Also known as ductal carcinoma in situ (DCIS), stage 0 always means that the cancer cells are found only inside the intact breast milk ducts.
Stage IA – T1, N0, M0
In this stage, the tumor measures up to 2 cm. It has become invasive with cancer cells spreading to normal tissue surrounding the tumor. It has not spread outside the breast, or if it is in nodes, the volume is less than 0.2mm and the node is still considered negative, and is designated thus: N0(i+).
Stage IB – T1, N1(mi), M0
The breast tumor is smaller than 2 cm. Small clusters of cancer cells are present in 1-3 lymph nodes in the armpit but are between 0.2mm and 2mm, and are designated with (mi), meaning micrometastatic. The cancer has not spread elsewhere.
Stage IB – T0, N1(mi), M0
This is invasive cancer in which there is no tumor identified in the breast, but cancer cells are present in 1-3 lymph nodes in the armpit. The cell clusters in the node(s) are between 0.2mm and 2mm and have not spread to other parts of the body.
Stage IIA – T0, N1, M0
This is invasive breast cancer, but there is no tumor in the breast. Cancer is present in 1-3 lymph nodes in the armpit or internal mammary nodes near the breastbone. The cancer has not spread elsewhere.
Stage IIA – T1, N1, M0
A breast tumor less than 2 cm is present. Cancer cells are also present in 1-3 lymph nodes in the armpit or the internal mammary nodes. The cancer has not spread elsewhere.
Stage IIA – T2, N0, M0
A breast tumor between 2-5 cm is present. There are no cancer cells in the lymph nodes. The cancer has not spread elsewhere.
Stage IIB – T2, N1, M0
A breast tumor between 2-5 cm is present. There are cancer cells in 1-3 lymph nodes or in the internal mammary nodes. The cancer has not spread elsewhere.
Stage IIB – T3, N0, M0
A breast tumor over 5 cm is present. No lymph nodes are involved. The cancer has not spread elsewhere.
Stage IIIA – T0-3, N2, M0
Whether or not there is tumor in the breast, cancer cells are present in 4-9 lymph nodes in the armpit or the internal mammary nodes. The cancer has not spread elsewhere.
Stage IIIA – T3, N1, M0
The breast tumor is over 5 cm. Cancer cells are present in 1-3 lymph nodes in the armpit or internal mammary nodes. The cancer has not spread elsewhere.
Stage IIIB – T4, N0-2, M0
There is a breast tumor of any size which has spread into the chest wall, invading the muscle or bone (T4a), or it has invaded the breast skin (T4b), or it invaded both chest wall and skin (T4c), or it is designated “inflammatory breast cancer” (T4d). Cancer cells are present in 0-9 lymph nodes in the armpit and/or internal mammary nodes. The cancer has not spread elsewhere.
Stage IIIC – Any T, N3, M0
There is a breast tumor of any size which has spread to 10 or more lymph nodes in the armpit or internal mammary nodes. Or it has spread to the nodes above the collarbone (“supraclavicular nodes”).
Stage IV – Any T, Any N, M1
The tumor may be any size and may or may not be in local lymph nodes, but it has spread to other organs, which most commonly include lymph nodes beyond the armpit and internal mammary area, bone, lung, liver, or brain.
 We’ve been working hard on this. Add your e-mail address and we will tell you as soon as it launches.
We’ve been working hard on this. Add your e-mail address and we will tell you as soon as it launches.
"*" indicates required fields
When you receive your breast cancer pathology report, you and your doctor will read through it and discuss the findings and how they affect your treatment options. Remember to ask if you need any other tests to give a clearer picture of your type of cancer. If you have just been diagnosed. Dr. Kristi Funk’s bestseller, Breasts: The Owner’s Manual provides an excellent and detailed guide to optimizing your treatment outcomes, and her book will become an invaluable resource to you with respect to life during and after treatment.